Everyone has heard about the importance of blood donation. However, not many people are aware of the equally important act of plasma donation. While both blood and plasma are used to save the lives of those who experience severe trauma, plasma’s uses are more specific.
According to the American Red Cross, nearly 10,000 units of plasma are needed in the United States every day. And one pint of donated plasma has the potential to save three lives!
Donating plasma is a wonderful way to help others while making some extra money, especially for those undergoing life changes that may require supplemental income, such as new parents.
Can you donate plasma while breastfeeding? Is it safe? Although there is no hard evidence that states donating plasma while nursing has any detrimental effects on the mother or the baby, the World Health Organization (WHO) advises against it.
Things to Know About Donating Plasma While Breastfeeding
-
Potential Side Effects of Donating Plasma While Nursing
According to the WHO, donating plasma while breastfeeding may cause side effects that can impact a mother’s milk supply. Plasma donation has the potential to lower electrolyte levels in the body which can lead to dehydration. Consequently, dehydration in a mother’s body can lead to low breast milk production.
Additionally, it is important to consider that the nutrients nursing mothers consume provide what they and their baby needs. However, there may not be enough nutrients in the mother’s system to be able to donate through their plasma.
The WHO advises waiting at least nine months from childbirth and three months after your baby is weaned from breast milk and is getting most of their nutrition from solid food or formula. Waiting for this period should allow your body ample time to recover, ensuring hemoglobin and iron levels are back to normal.
It appears, however, that donating plasma while nursing may be a personal choice. If you choose to donate plasma while breastfeeding, always consult your physician first, since your ability to donate may need to be evaluated on a case-by-case basis.
Whether you choose to donate plasma while nursing or after the suggested waiting period, the information below will be useful in helping you prepare for it.
-
What is Plasma?

Plasma is the protein-rich, pale, yellow fluid portion of blood that carries red and white blood cells, platelets, electrolytes, proteins, sugars, fats, hormones, and vitamins. It is about 92% water, and it makes up approximately 55% of blood.
Plasma helps maintain healthy blood pressure, blood volume, and proper pH level in the body, which helps cell function. It is also important in supporting blood clotting and in immune system responses. Additionally, the electrolytes in plasma help muscles function properly.
-
Why Donate Plasma
According to DonatingPlasma.org, donated plasma is used to create therapies that can treat rare diseases and chronic conditions. Additionally, plasma is used on individuals who experience severe trauma, burn, or shock.
Because its clotting ability can stop excessive bleeding, plasma is used on cancer patients experiencing complications where their body has used all their natural clotting factors. In such instances, plasma transfusion becomes critical.
-
Plasma Donating Criteria
If you are a nursing mother and decide to donate plasma, it is imperative you inform the donation center personnel of your situation.
When pregnant, blood cells from the baby mix with the mother’s blood through the placenta. In order to suppress the mother’s immune system enough to keep it from attacking the “foreign” matter in her body, it releases a protein called human leukocyte antigens (HLA).
While this process is perfectly normal and safe for both baby and mother, during a transfusion of your plasma to another person, the HLAs present in it can cause life-threatening complications to the recipient. Therefore, it is important to get tested for HLA before donating your plasma.
Every country has differing rules for nursing mothers, and not all donation centers have the same acceptance criteria. However, most agree on a variation of the following:
- Donor must be generally in good health, pass a medical exam, and complete a medical history screening
- Plasma donor must be between 18-65 years old
- Donor must weigh more than 110 pounds (50 kilograms)
- Donor must have had no tattoos or piercings in the past six months
- If the donor has had a miscarriage or terminated a pregnancy, she must wait six weeks (in some countries 12 weeks) to donate
Do not donate plasma if you have a cold, flu, sore throat, stomach virus, or other infection, if you have traveled to areas where mosquito-borne infections are common, or if you’ve had unprotected sex within the past 12 months.
Never donate plasma if you have tested positive for HIV (AIDS virus), have injected recreational drugs or steroids, or have a congenital blood clotting condition.
Do not donate plasma while pregnant, as it could cause undue stress on you and your baby.
-
Preparing Your Body to Donate Plasma

In the days leading up to your plasma donation, be sure to eat healthy, balanced meals. Eat a diet high in protein and iron, and low in fat. Greasy foods may affect the quality of your plasma.
If you want to donate plasma while breastfeeding remember to drink plenty of water, ideally 6-8 cups the day before you donate. Breastfeeding mothers require extra fluids to produce milk. Plasma donation further removes water from your body. Therefore, do not drink alcohol or caffeine as they are diuretics, and they may further dehydrate you.
Also, avoid tobacco before plasma donation.
-
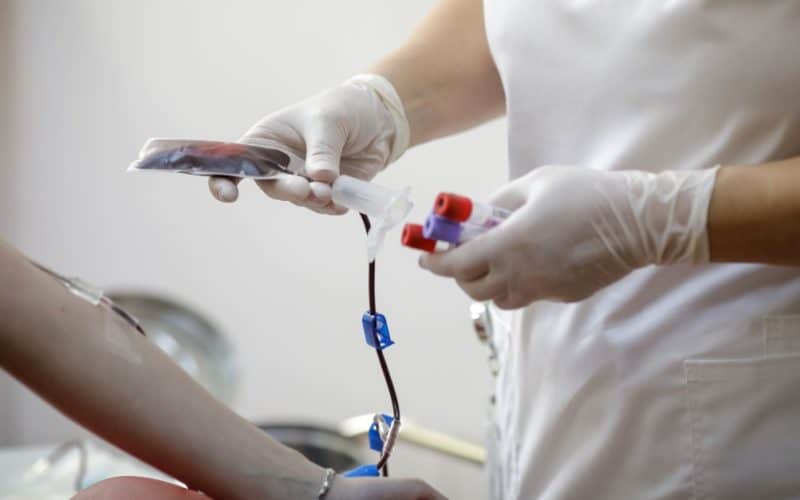
What to Expect During Plasma Donation
Plasma donation is very similar to blood donation. The main difference lies in the separation of the plasma from your blood.
Initially, the blood is drawn from your arm. The blood components are then separated through an automated process (the plasma goes into a bag). Finally, the remaining blood (red blood cells and platelets) goes back into your arm with a small amount of saline solution.
After your donation, you should have a snack and drink some fluids, usually provided by the donation center. Avoid lifting heavy objects or strenuous activities for the remainder of the day
The entire process takes one to two hours, including paperwork, health screening, and donation.
-
A Nursing Mother’s Alternatives to Donating Plasma
If you decide to heed the WHO’s recommendations to wait before donating plasma, but still would like to help your community in some way, you may consider cord blood donation or breast milk donation.
Cord Blood
Cord blood is found inside the placenta and umbilical cord and can be donated at your request, immediately after delivery. According to the United States Food and Drug Administration (U.S. FDA), “Cord blood contains hematopoietic progenitor cells (HPCs)” which “are blood-forming stem cells.”
The stem cells found in the cord blood can be used to treat many conditions, including leukemia, lymphoma, and sickle cell disease.
Breast Milk
By donating your excess breast milk to donor banks, you may help fragile, premature babies in hospitals as well as families with infants in need. According to the Milk Banking Association of America, “donor milk is collected from qualifying donors, screened, pooled, and then pasteurized so it is safe for use.”
So, Can You Donate Plasma While Breastfeeding?
Although there is no concrete evidence of any harmful effects on nursing mothers or their babies by donating plasma, the WHO recommends a waiting period before donating. Despite plasma donation being an altruistic endeavor, mothers must take into consideration that doing so may deplete their breast milk supply due to dehydration.
Ultimately, it is up to the mother and her physician to decide whether donating plasma while breastfeeding is a healthy choice for her.